17
Mar
Joint Replacement Surgery
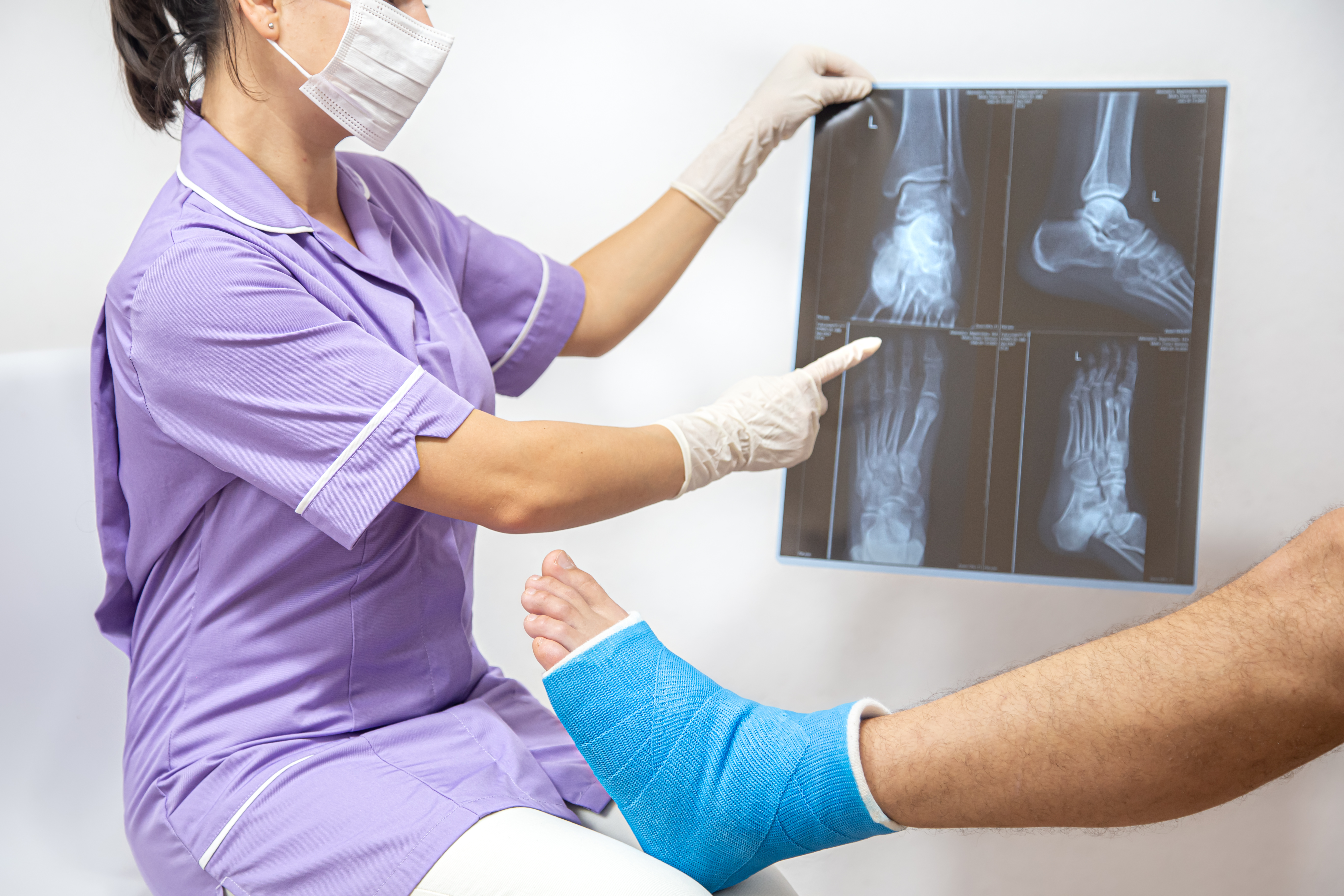
When You Need Revision Joint Replacement Surgery: A Guide for Patients in Hyderabad
Total knee replacement and hip replacement surgeries have long been hailed as some of the most successful and life-changing procedures in modern orthopedic medicine. For millions of people, these surgeries mean the difference between chronic pain and active, painless mobility. As life expectancy increases and the demand for a high quality of life in our later years grows, the number of primary joint replacement procedures has increased exponentially over the past decade.
However, with a greater number of people living longer with artificial joints, a new challenge has emerged: Revision Joint Replacement. While a primary joint replacement is designed to last for 15 to 20 years or more, various factors can lead to the need for a second surgery. At Olive Hospital, Hyderabad, we believe that understanding this process is key to ensuring long-term mobility and health.
Revision Joint Replacement: An Emerging Challenge
In the past, there was a common misconception that once a joint replacement failed, a patient's options were limited, often leading to permanent pain and immobility. Today, that narrative has changed completely. Thanks to significant advancements in surgical techniques, implant design, and specialized medical expertise, failed joints can now be successfully salvaged. The key to a successful outcome, however, lies in timely diagnosis.
Revision surgery is inherently more complex than a primary replacement. It involves removing the old, worn-out, or failed implant and inserting a new one. This procedure requires a higher level of skill because the surgeon must work with compromised bone stock, scar tissue, and the need to remove old cement or components. At our facility in Hyderabad, we are equipped with the latest technology to meet these challenges head-on, ensuring that a failed joint is no longer an endpoint, but a detour on the road to recovery.
Common Causes of Joint Replacement Failure
Joint replacements are incredibly durable, but they are not indestructible. Understanding why a replacement might fail is the first step in prevention and early intervention. The failure of a well-performed joint replacement can typically be attributed to one of several factors:
- Infection: This is one of the most serious complications. An infection can occur shortly after the surgery or even years later, as bacteria from other parts of the body travel through the bloodstream and settle around the implant.
- Aseptic Loosening: This is the most common cause of long-term failure. It refers to the gradual loosening of the implant from the bone over time, without the presence of infection. This can be caused by wear particles from the implant (such as polyethylene debris) that cause the body to resorb bone around the implant.
- Instability or Dislocation: Sometimes, the joint may become unstable, leading to a feeling of "giving way" or, in the case of hips, actual dislocation. This can result from ligament imbalance or wear and tear of the soft tissues surrounding the joint.
- Fracture (Periprosthetic Fracture): A fall or trauma can cause the bone around the implant to break. This is known as a periprosthetic fracture and often requires surgery to stabilize the bone and replace the implant.
- Implant Wear and Breakage: While modern implants are designed to withstand immense force, mechanical wear over decades can lead to the implant breaking or the polyethylene liner wearing thin.
Among these, infection and aseptic loosening are the most significant and demand timely management to prevent further damage.
Early Signs of Implant Failure: Listen to Your Body
Your body often sends clear signals when something is wrong with your joint replacement. Ignoring these warning signs can lead to more complex problems down the line. You should consult a specialist at Olive Hospital if you experience any of the following:
- Pain on Startup: Experiencing sharp pain when you first stand up or start walking, which may ease after a few steps, can be an early indicator of loosening.
- New or Worsening Pain: Pain that was not present in the years following your surgery, especially pain that wakes you up at night or is persistent at rest, is a red flag.
- Limping: Developing a new limp or finding it increasingly difficult to walk without a limp.
- Feeling of Instability: A sensation that the joint is going to "give out" or buckle under you.
- Need for Walking Support: If you suddenly need a cane or walker after years of walking independently, it signals a problem.
- Abnormal Sounds: Grinding, clicking, or squeaking noises coming from the joint can indicate wear and tear.
- Reduced Range of Motion: If you notice it is becoming harder to bend or straighten the joint, or if it feels stiffer than before.
- Swelling, Warmth, or Redness: These are classic signs of inflammation and could indicate infection or an inflammatory reaction to wear debris.
These warning signs should never be ignored. Early consultation is the most critical step in preserving your bone and ensuring a successful revision.
The Importance of Early Evaluation and Diagnosis
If you are experiencing any of the symptoms above, a prompt consultation with an orthopedic surgeon is essential. At Olive Hospital, Hyderabad, our diagnostic process is thorough and designed to pinpoint the exact cause of the failure. The evaluation may include:
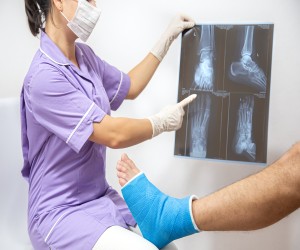
- X-rays: These are the first line of imaging. They can show loosening, bone loss, fractures, or changes in the position of the implant.
- Blood Investigations: Blood tests, including Complete Blood Count (CBC), Erythrocyte Sedimentation Rate (ESR), and C-Reactive Protein (CRP), are crucial for detecting inflammation or infection.
- Advanced Imaging: An MRI or a CT scan can provide a more detailed view of the bone stock, the integrity of the soft tissues, and the exact extent of bone loss, which is vital for pre-surgical planning.
- Joint Fluid Aspiration: If infection is suspected, a sample of fluid from the joint may be drawn (aspirated) and sent to a lab to culture and identify any bacteria.
Early and accurate diagnosis is the foundation of effective treatment. It allows the surgical team to plan the appropriate management strategy, whether it is conservative treatment or a complex revision.
Conservative Management vs. Revision Surgery
Not every case of post-surgical discomfort requires immediate revision. In some instances, conservative measures may suffice. This could include physical therapy to strengthen surrounding muscles, activity modifications, or pain management strategies.
However, when diagnostic tests confirm loosening, infection, or implant failure, revision surgery should not be unnecessarily delayed. There is a harmful misconception that one must "wait as long as possible" before getting a revision. This is simply not true.
“Time is Bone”: Why Early Intervention Matters
In revision joint surgery, a fundamental principle guides every decision: "Time is Bone." Bone is the foundation upon which the new implant will rest. If you continue to walk on a loosened implant, the constant movement and friction can grind away the existing bone. This leads to:
- Significant Bone Loss: The femur, tibia, or acetabulum (hip socket) can lose critical mass, making it difficult to seat a new implant.
- Complex Reconstructions: Surgeons may need to use bone grafts (from a donor or cadaver) to rebuild the lost bone structure.
- Need for Specialised Implants: Significant bone loss may require very large, specialized, or custom-made revision implants, which are more expensive and complex to implant.
- Increased Surgical Complexity and Risk: The more bone that is lost, the more complicated the surgery becomes, increasing the risk of complications like fracture during surgery.
Early, precise, and focused intervention is not just about fixing the joint; it is about preserving your biology to ensure the best possible long-term outcome.
Single-Stage Revision in Non-Infective Cases
In cases where infection has been ruled out (aseptic loosening), the revision can often be performed as a single-stage procedure. This means the entire surgery-removing the old implant and placing the new one-is done in one operation.
Using specialized revision implants designed to bypass damaged bone areas and achieve a stable fit, a skilled surgical team can achieve outcomes that are comparable to a primary joint replacement. This approach minimizes the time a patient spends in the hospital and allows for a faster, more streamlined recovery process. At Olive Hospital, our surgeons utilize meticulous planning and advanced techniques to ensure the success of these complex single-stage revisions.
The Role of Technology and Robotics in Revision Surgery
The field of orthopedics has been transformed by technology, and this is especially true for complex procedures like revision surgery. Robotic-assisted surgery is particularly helpful in revision cases for several reasons:
- Navigating Distorted Anatomy: After a primary surgery, the normal bony landmarks a surgeon relies on are often distorted due to bone loss, implant removal, and scar tissue. Robotic systems provide real-time, 3D mapping of the patient's unique anatomy, allowing the surgeon to navigate this complex landscape with incredible precision.
- Accurate Implant Placement: The robot assists the surgeon in executing the pre-operative plan with pinpoint accuracy, ensuring that the new implant is placed in the optimal position for stability and long-term survival.
- Minimizing Trauma: By enhancing precision, robotic assistance can help protect the remaining healthy bone and soft tissues, leading to better outcomes.
Two-Stage Revision for Infected Cases
When infection is the cause of failure, the surgical approach is different. Treating an infected joint replacement requires eradicating the bacteria before a new implant can be safely placed. This usually involves a two-stage revision:
- First Stage: The surgeon removes the old infected implant, performs a thorough and meticulous cleaning of the joint (a debridement), and places a temporary spacer made of antibiotic-infused cement. This spacer helps maintain joint space and delivers high doses of antibiotics directly to the area. The patient is then treated with a course of intravenous or oral antibiotics for several weeks.
- Second Stage: Once the infection has been cleared-confirmed by blood tests and absence of clinical signs-the patient returns for the second surgery. The spacer is removed, and the new, permanent revision implants are placed.
Modern surgical techniques and advanced antibiotics have greatly improved the success rates of two-stage revisions, allowing patients to overcome this challenging complication and return to a pain-free life.
The Rising Challenge of Atypical Infections
The medical community is increasingly recognizing the challenge posed by atypical infections. These are infections caused by bacteria or fungi that are less common and harder to identify with standard cultures. They can be indolent (slow-growing) and present a long-term management challenge. However, ongoing advances in microbiological research, including techniques like PCR and next-generation sequencing, are improving our ability to detect these organisms. Coupled with the development of newer, more potent antibiotics, we are steadily improving infection control and outcomes for patients facing these difficult diagnoses.
Conclusion: Revision Surgery is a Solution, Not a Limitation
The landscape of revision joint replacement has evolved dramatically. What was once a feared and often avoided procedure is now a highly successful solution for restoring mobility and eliminating pain. The key takeaways for anyone living with a joint replacement are clear: listen to your body, do not ignore the early signs of failure, and seek expert consultation promptly. Remember the mantra "Time is Bone" -early intervention is your best ally.
At Olive Hospital in Hyderabad, we are at the forefront of this specialized field. Our team of experienced orthopedic surgeons is equipped with the latest technology, including robotic assistance, to handle the most complex revision cases. We are committed to providing personalized care, from accurate diagnosis and meticulous surgical planning to comprehensive post-operative rehabilitation.
If you are experiencing pain, instability, or any other concerning symptoms in a replaced joint, do not wait. Revision surgery is no longer a limitation; it is a pathway back to the active, painless life you deserve. Contact Olive Hospital, Hyderabad, to schedule a consultation and take the first step toward reclaiming your mobility.
Frequently Asked Questions (FAQs) About Revision Joint Replacement
- How long does a revision joint replacement last?
While primary joint replacements are designed to last 15-20+ years, the longevity of a revision is more variable and depends on several factors, including the reason for the revision, the amount of bone loss, the type of implant used, and the patient's activity level. Generally, with modern techniques and implants, patients can expect a revision to last for many years, though possibly not as long as a primary replacement. - Is revision surgery more painful than the first replacement?
The post-operative pain experience can vary. Because revision surgery is more invasive and involves cutting through scar tissue and working with compromised bone, the initial recovery might be more uncomfortable. However, modern pain management protocols, including multimodal analgesia and nerve blocks, are highly effective at controlling pain. The long-term goal is the same: to eliminate the pain caused by the failing implant. - What is the recovery time for a revision joint replacement?
Recovery from revision surgery is generally slower and more cautious than from a primary replacement. Patients may need to use a walker or cane for a longer period (often 6 weeks or more) to protect the bone and allow the new implant to integrate. Physical therapy is crucial, but the timeline for returning to specific activities will be tailored to the individual and the complexity of the surgery. - Can a revision be done with robotic assistance at Olive Hospital, Hyderabad?
Yes. Olive Hospital in Hyderabad is equipped with advanced robotic technology for joint replacement surgeries. Robotic assistance is particularly valuable in revision cases, as it allows for greater precision in navigating distorted anatomy and achieving optimal placement of complex revision implants, which can lead to better outcomes. - What happens if my revision surgery fails?
While rare, a revision can fail. The options depend on the cause of failure. It could involve another revision surgery (making it a third replacement), which is even more complex. In extreme cases with massive bone loss and poor soft tissue, other options like joint fusion (arthrodesis) or, in very select cases, amputation might be considered, though these are absolute last resorts. Your surgeon will discuss all possible scenarios and long-term plans.